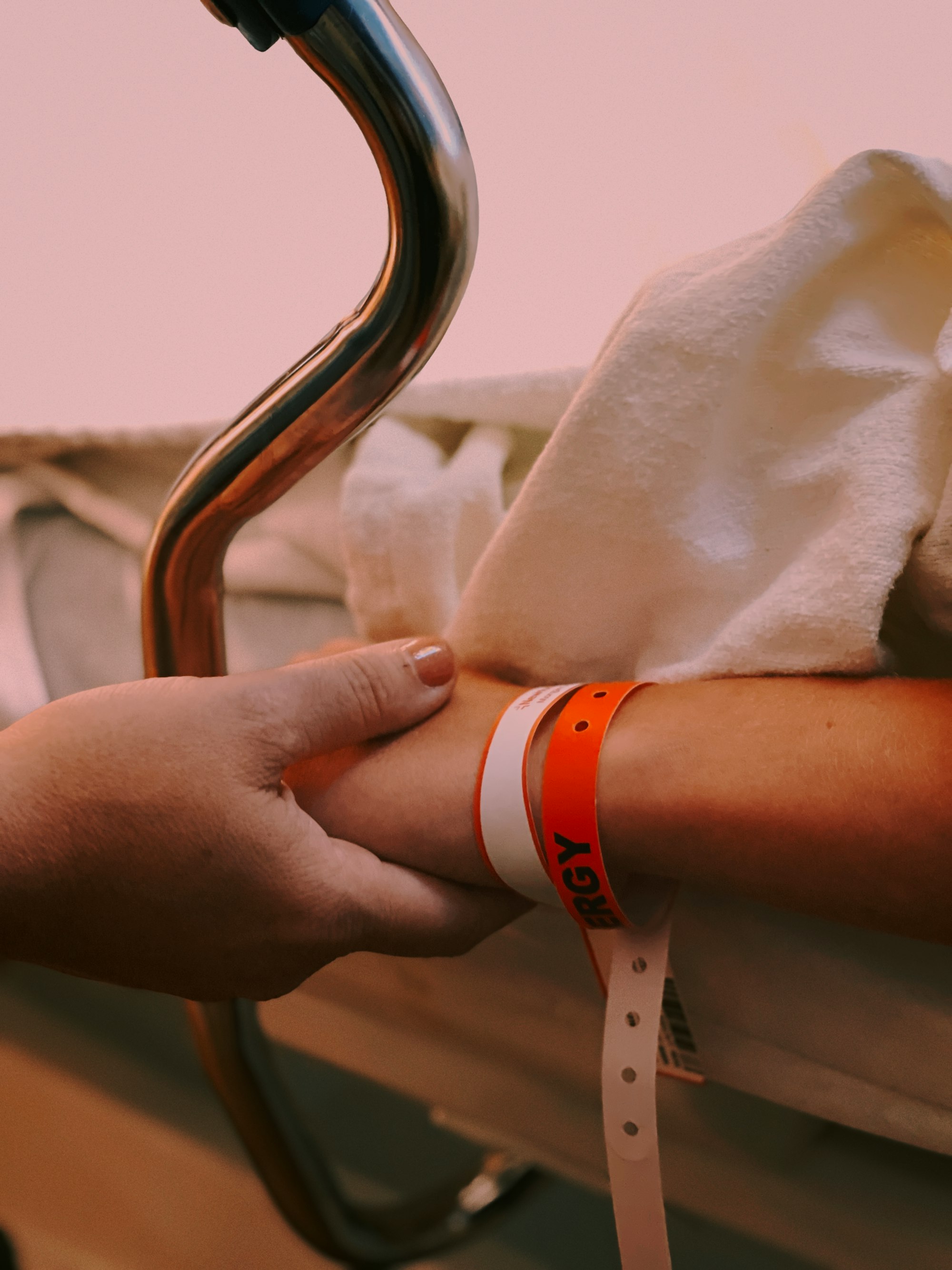
Comprehensive Guide to Managing Toileting and Incontinence in Dementia Care
Explore a comprehensive guide to navigating toileting and incontinence in dementia care. Learn to manage these sensitive issues with dignity, from recognizing early signs to adopting effective strategies for hygiene, environmental adaptations, and empathetic communication.

Understanding Incontinence in Dementia
Incontinence, or the loss of bladder and bowel control, is a common issue in dementia care. It's a sensitive and challenging aspect for caregivers and family members, often emerging as dementia progresses.
Defining Incontinence
- Urinary Incontinence: Involves the inability to control urine flow, often starting at night and eventually spreading to daytime hours.
- Fecal Incontinence: Loss of bowel control, leading to involuntary defecation, which may follow urinary incontinence.
Early Signs and Prompt Responses
In early-stage dementia, individuals might need reminders for bathroom use. Simple aids like signs or symbols leading to the bathroom can be helpful.
Recognizing Early Indicators
- Behavioural Cues: Restlessness, clothing tugging, or pacing may indicate a need for toileting.
- Physical Symptoms: Watch for signs that might suggest conditions like urinary tract infections, which can exacerbate incontinence.
Strategies for Managing Daytime Incontinence
Effective management involves a combination of routine, environmental adaptations, and empathetic care.
Establishing a Routine
- Scheduled Bathroom Breaks: Encourage bathroom visits every two hours to prevent accidents.
- Recognition of Needs: Pay attention to non-verbal cues indicating the need to use the toilet.
Creating a Supportive Environment
- Accessibility: Ensure the toilet is easily accessible, with clear pathways.
- Safety Features: Install grab bars and use non-slip mats to enhance safety.
Clothing Considerations
- Ease of Dressing: Choose clothes that are easy to remove, like those with elastic waistbands, to simplify toileting.
Managing Nighttime and Public Incontinence
Addressing incontinence effectively during the night and in public settings requires additional planning.
Nighttime Strategies
- Bedside Solutions: Consider a portable commode or bed pads.
- Fluid Intake: Limit liquids in the evening to reduce nighttime bathroom trips.
Out and About
- Preparation: Plan for accessible bathroom locations and carry spare clothing and incontinence products.
Tips on How to Get Them To Sit on the Toilet
Addressing Incontinence with Compassion
Approach accidents with understanding and patience. Maintain dignity and privacy during care.
Hygiene and Skin Care
- Regular Cleaning: Gently wash the skin after incontinence episodes.
- Barrier Creams: Use to protect skin from moisture.
Absorbent Products
- Selecting the Right Products: Choose appropriate pads or adult diapers for absorbency and comfort.
- Regular Changes: Change incontinence products promptly to maintain skin health.
Incontinence and Diet
Dietary choices can impact bladder and bowel health.
Dietary Tips
- Avoid Irritants: Steer clear of caffeine, carbonation, and spicy foods.
- Fiber Intake: Include fiber-rich foods to prevent constipation.
- Hydration: Aim for 6-8 glasses of water daily while balancing fluid intake to manage incontinence.
Professional Support and Care
Seeking medical advice is crucial for proper management.
Medical Consultation
- Regular Check-Ups: Report any changes in incontinence patterns.
- Comprehensive Reporting: Provide detailed information on the type, severity, and timing of incontinence episodes.
Collaborating with Health Professionals
- Nursing Support: For hygiene management advice.
- Physical Therapy: For equipment and mobility adaptations.
Navigating Incontinence in Dementia Care
Managing incontinence in dementia requires an informed, empathetic approach. Understanding the challenges, adopting practical strategies, and maintaining dignity are key to effective care. By staying attentive to the needs and providing compassionate support, caregivers can greatly enhance the quality of life for individuals with dementia.

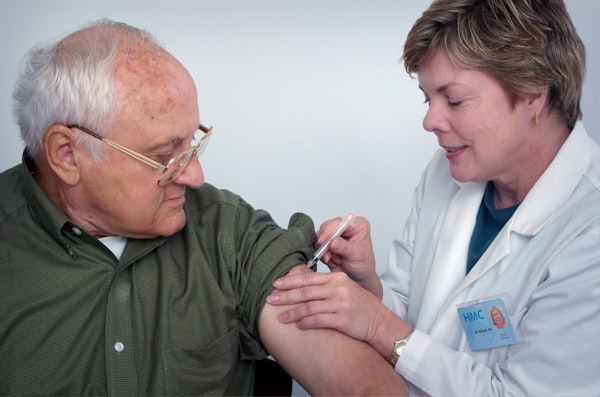
Recognizing Urinary Tract Infections in Dementia: Impact on Incontinence and Confusion
Introduction: UTIs and Their Significance in Dementia Care
Urinary Tract Infections (UTIs) are common among the elderly, especially those with dementia. Recognizing the signs and symptoms of UTIs is crucial, as they can exacerbate incontinence and cause increased confusion.
Understanding UTIs in the Elderly with Dementia
UTIs occur when bacteria enter the urinary tract, leading to infection. They can have a more pronounced impact on individuals with dementia due to their reduced ability to communicate symptoms.
Common Symptoms of UTIs
- Increased Frequency of Urination: An urgent need to urinate more often.
- Burning Sensation During Urination: Discomfort or pain while urinating.
- Cloudy or Bloody Urine: Changes in the appearance or smell of urine.
- Fever or Chills: Indicating the body's response to infection.
- Pelvic or Lower Back Pain: Discomfort in the lower abdomen or back.
Symptoms Specific to Dementia Patients
- Worsening Confusion: Sudden or increased confusion can be a key indicator.
- Agitation or Irritability: Changes in behavior or mood.
- Decreased Mobility or Falls: UTIs can lead to weakness or unsteadiness.
- Increased Incontinence: A noticeable increase in urinary incontinence episodes.
The Link Between UTIs, Incontinence, and Confusion
UTIs can significantly affect individuals with dementia, leading to increased incontinence and confusion, which are often mistaken for the progression of dementia.
Exacerbation of Incontinence
- Overactive Bladder: UTIs can irritate the bladder, causing more frequent and urgent urination.
- Loss of Control: The infection can lead to a temporary loss of bladder control.
Impact on Cognitive Function
- Delirium: UTIs can cause acute confusion or delirium, which can be mistaken for a sudden worsening of dementia.
- Disorientation: Patients may appear more disoriented and have difficulty with communication.
Managing UTIs in Dementia
Prompt recognition and treatment of UTIs are essential to prevent complications and minimize their impact on incontinence and cognitive function.
Diagnosis and Treatment
- Medical Evaluation: Consult a healthcare provider for proper diagnosis and treatment, typically involving antibiotics.
- Hydration: Ensure adequate fluid intake to help flush out the infection.
Preventive Measures
- Personal Hygiene: Maintain good hygiene to reduce the risk of UTIs.
- Regular Bathroom Breaks: Encourage frequent toileting to prevent urine retention.
- Cranberry Juice or Supplements: May help in preventing recurrent UTIs, though consult with a healthcare provider first.
Conclusion: Importance of Vigilance in UTI Symptoms
In individuals with dementia, UTIs can lead to significant changes in incontinence and cognitive function. Being vigilant about the symptoms and seeking timely medical intervention is crucial. Understanding these connections can aid caregivers in providing effective care and preventing further complications associated with UTIs.
Frequently Asked Questions:
When does incontinence occur in dementia?
Incontinence typically develops in the middle-to-late stages of dementia, although this can vary.
Why do dementia patients experience incontinence?
Possible reasons for incontinence in dementia patients include loss of bladder or bowel control, difficulty recognizing the need to use the toilet, communication issues, inability to reach the bathroom in time, and mobility loss. In some cases, accidents can lead to embarrassment and potentially contribute to depression.
What are signs of worsening dementia?
The progression of dementia varies from person to person, but it generally involves:
Initial confusion and minor misplacements of items
Increased need for assistance with daily tasks, including self-care and possible personality changes
Transition to requiring full-time care and loss of independence.
More on Dementia and Incontinence at home...
Assisting your loved one with their ADLs can be physically taxing. And emotionally draining, Especially in the later course of the disease.
These sections on activities of daily living are to help provide you with an “edge”. These dementia tips and strategies will decrease problematic occurrences. And increase your caregiving efficiency. And in doing so, you and your family member will benefit.
Here are some other tips that you may find useful when providing ADL’s :
- Eating
- Toileting
- Ambulation
- Bathing
- Dressing
- Personal Care
- Transferring
- Cooking
- Shopping
- Medication management
- Managing finances
- Housework
- Laundry
You might also like this article: