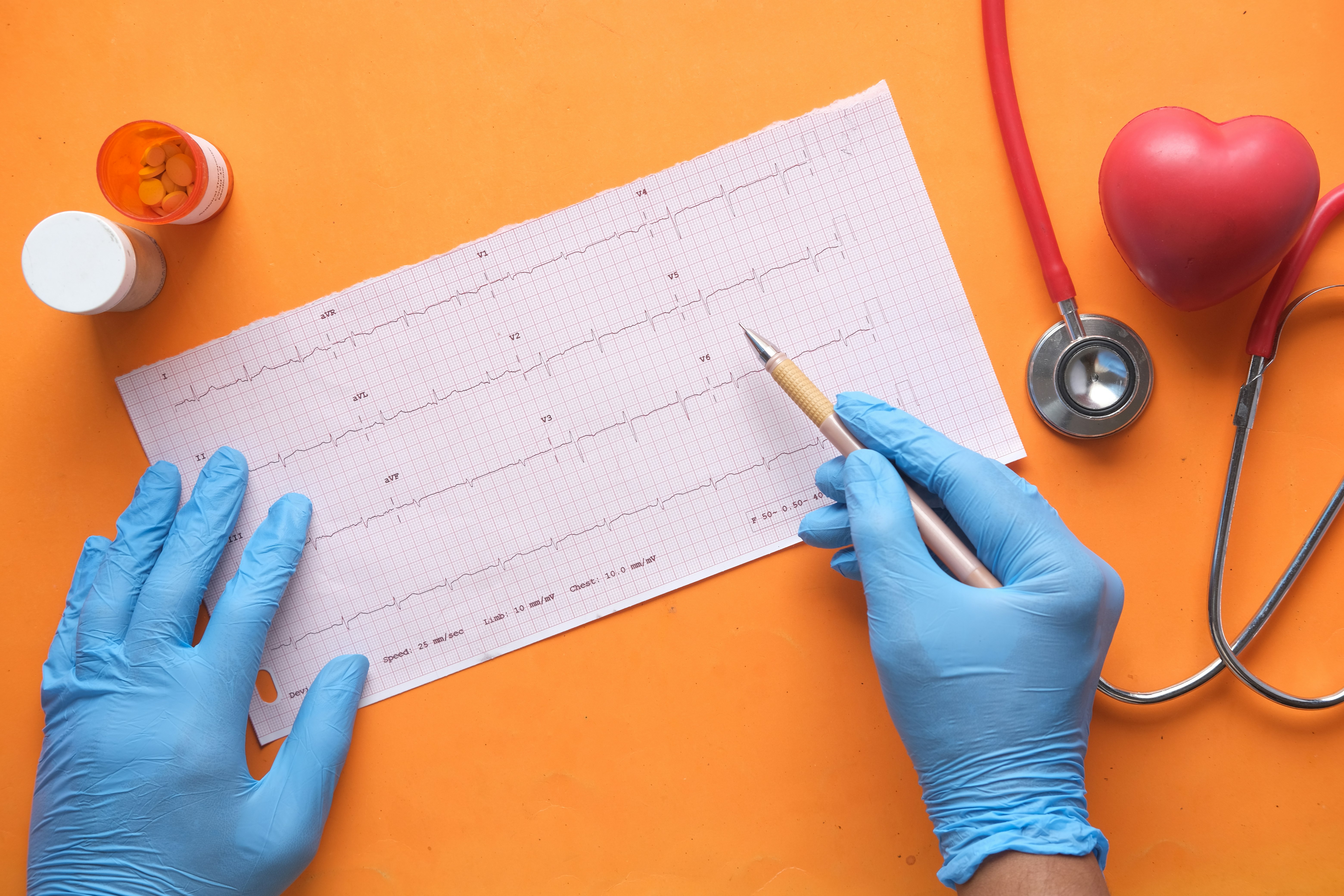
Is Palliative Care the Same as Hospice?

Understanding the difference between palliative care and hospice care is an important step in making sure that end-of-life decisions are based on accurate information. Palliative care and hospice care are both methods of providing comfort and relief from the symptoms of a terminal illness. While there are similarities between the two, they also have crucial differences that are important to understand.
Palliative care is a type of medical care that focuses on relieving the physical, emotional and spiritual distress caused by a serious or life-limiting illness. It is usually recommended when the patient is facing a complex or serious health condition and aims to improve their quality of life while living with their illness. Hospice care, on the other hand, is a type of care designed for people who have a terminal illness and have been given six months or less to live. Hospice is generally recommended when there is no longer any benefit to be gained from medical treatments and the primary focus of care becomes comfort, peace and dignity.
With these two types of end-of-life care, it can be difficult to make sure you’re selecting the right one, so it’s important to have a thorough understanding of the differences between the two. In this guide, we’ll cover the details of palliative care, hospice care, advanced care planning, and more to help you make the best decision for yourself or a loved one.
What is Palliative Care?
Palliative care is a type of medical care for those who have a serious illness. It is focused on providing relief from the symptoms, pain, and stress of a serious illness—whatever the diagnosis. The goal of palliative care is to improve quality of life for both the patient and the family. Palliative care is provided by a team of doctors, nurses, and other specialists who work together with a patient's other doctors to provide an extra layer of support. It is appropriate at any age and any stage in a serious illness, and it can be provided alongside curative treatment.
When Is Palliative Care Suggested?
Palliative care is usually suggested when a person has a serious or life-threatening illness such as cancer, heart failure, dementia, or any other condition that causes significant distress. Palliative care can also be beneficial for people who are undergoing treatments like chemotherapy or radiation. It is often suggested when the goals of care shift from curing the illness to managing symptoms and improving quality of life.
How Can Palliative Care Help Patients and Their Families?
Palliative care provides a supportive environment where a patient can discuss their concerns and make decisions about their care. This type of care focuses on relieving physical symptoms such as pain, nausea, breathlessness, and fatigue. It also helps with emotional, spiritual, and practical issues.
Palliative care can help families by providing guidance on how to best support their loved one. It helps to create a plan for long-term care and offer advice on navigating difficult conversations. Additionally, palliative care teams can provide emotional support for families during this difficult time.
Detailed Information About Hospice Services
Hospice care and palliative care offer different types of end-of-life care that are tailored to the patient’s needs and desired level of support. While both types of care provide comfort and relief for those nearing the end of life, there are some important differences between the two.
Palliative care focuses on managing the physical, psychological, and social symptoms of a person’s illness—regardless of their diagnosis or prognosis. Whereas, hospice care is available for people who may be in the last stages of their illness and when curative treatments are no longer beneficial. Hospice focuses on providing emotional and spiritual support for not only the patient, but also their family members and loved ones.
Hospice is typically recommended when a patient’s doctor believes that they have six months or less to live. In addition to addressing physical symptoms, hospice works to improve the quality of life for terminally ill patients by significantly reducing suffering, providing emotional and spiritual support, and honoring end-of-life wishes. Hospice also offers providers who specialize in pain and symptom management, as well as comprehensive resources that address the physical, social, and spiritual needs of both the patient and their family.
The key difference between palliative care and hospice care is that hospice provides more specialized services in addition to comfort care. Hospice teams consist of professionals from many healthcare disciplines, including physicians, nurses, social workers, spiritual counselors, and volunteers who work together to provide the best care possible for the patient and their family.
Advanced Care Planning for Terminally Ill People
When facing a terminal illness, advanced care planning is an important step to consider. It involves creating a written plan with your doctor and family members that outlines your end-of-life wishes. Advanced care planning can help make sure that your loved ones understand your wishes and provide you with the right care.
The process of advanced care planning begins with talking to your doctor. Your doctor can discuss all the possible treatment options available for your illness, and explain the potential benefits and risks of each. They can also help you decide which care would best address your individual needs. With this knowledge, you can then make an informed decision on the type of care that you prefer as well as the level of care that you want in the future.
It is also important to involve family members in your plan. They can provide valuable insight and advice into what you want for the end of your life. Their input can also be a great source of support during this difficult time. Additionally, they can serve as an advocate for your wishes if you become unable to express them.
The next step is to create a written document outlining your wishes. This document should include all of the important details regarding the type of care you want to receive and any specific treatments or procedures you may want to avoid. It can also include instructions about medical decisions such as resuscitation and artificial nutrition, as well as information about who should be contacted in the event of an emergency.
Finally, you should ensure that your wishes are respected by signing an advanced directive. An advanced directive is a legal document that states your preferences for medical care and other end-of-life decisions. It should be signed by both you and your doctor in order for it to be legally binding.
Advanced care planning can be an overwhelming process, but it is important to take the time to explore all of your options. With careful thought and planning, you can ensure that your wishes are respected and that you receive the care you need.
Benefits of Palliative and Hospice Care
Palliative and hospice care are an important part of end-of-life care. They can provide immense physical, emotional, and spiritual support for those facing terminal illnesses. Patients and their families have access to an interdisciplinary team of physicians, nurses, social workers, counselors, and volunteers who can create a holistic approach to care.
Both palliative and hospice care recognize the importance of providing comfort and dignity to those in their last days. Through palliative care, patients can reduce pain and improve the quality of life through symptom management. Hospice care provides emotional and spiritual support through the entire process and emphasizes patient autonomy and respect for personal wishes.
The benefits of palliative and hospice care extend beyond the patient. Caregivers often require support during this difficult time and palliative and hospice care provide access to resources and programs that can help them better understand how to provide physical and emotional care to their loved one.
Questions to Ask a Doctor About Palliative and Hospice Care
Taking the time to understand and ask questions about palliative and hospice care before making a decision is very important. Before deciding on a course of action, it's a good idea to bring up these important topics with your doctor.
- What type of end-of-life care is best for my or my loved one's individual needs?
- What benefits does palliative care provide?
- What might I expect from a hospice program?
- What are my options for pain and symptom management?
- What kind of access will I or my loved one have to specialist services?
- How will I or my loved one be able to connect with friends and family?
- What do I need to know about CPR and do-not-resuscitate orders?
- Where can I find more information about advanced care planning?
- What resources are available for caregivers?
- When faced with a terminal illness, the patient and their loved ones may worry about the amount of discomfort and suffering they will experience. Fortunately, there are a number of strategies to increase comfort and prolong happiness during the end of life.
- The most important thing a patient facing a terminal illness can do is to actively participate in their treatment plan. Patients should collaborate with their healthcare team to identify an approach that works best for them. This could include adopting lifestyle changes like limiting activities or engaging in light exercise as recommended by a physician.
- Additionally, many patients find that managing pain levels makes a big difference in their quality of life. Taking medications and giving up certain activities can help keep pain under control. It is also important to have an understanding of the potential side effects of the treatments so that family members can watch out for any potential issues.
- During this difficult time, it is important to remember that life is still worth living. While the patient might need to make some adjustments to their daily routine, they can still make time for the activities that bring them joy. A patient may be able to travel or visit a place of spiritual significance. As long as they take the necessary precautions, it may be possible to enjoy a range of activities like listening to music, going for walks, or spending time with friends and family.
- Patients should also turn to their faith for comfort. Those who are religious can visit a place of worship, seek counseling from their clergy, or talk to a spiritual advisor. A spiritual or faith-based approach to treatment can be a powerful source of strength in difficult times.
- Terminal illnesses can be overwhelming and cause fear and anxiety. However, by taking an active role in their treatment plan and finding joy in small things, patients can help maintain their quality of life. It is essential to seek help from family members, medical professionals, and spiritual advisors in order to ensure the most comfortable end-of-life journey possible.
- When someone is nearing the end of life, there are many difficult decisions to make, including whether or not to opt for cardiopulmonary resuscitation (CPR). CPR is a medical procedure used to restart the heart and lungs in the event of a cardiac arrest. It is also possible to create a do-not-resuscitate order (DNR) that prevents any such resuscitation attempts from being made. Determining whether or not to have a CPR or DNR can be a difficult conversation to have, but it is an important one to consider when discussing end-of-life care.
- When it comes to CPR and DNRs, the patient and/or their medically authorized representative has the final say on whether or not they should be attempted. It is important for all involved to discuss, reflect on, and thoroughly understand the potential risks and benefits of both CPR and DNR before deciding on the best course of action. Depending on a person’s prognosis, CPR may be seen as a riskier option, as it can cause further damage to the body and increase pain and suffering for the patient. On the other hand, opting for a DNR means that the patient will not be able to benefit from any potential medical advancements that could help prolong their life.
- CPR and DNR orders can have a major impact on end-of-life decisions, so it is important to weigh your options carefully and to take into account the wishes and opinions of the patient and/or their medical representative. Ultimately, the decision should be based on the individual circumstances of the patient.
Cardiopulmonary Resuscitation (CPR) and Do-Not-Resuscitate Orders (DNRs)
Conclusion
Finding Joy in Life
Adopting Strategies for Comfort
Focusing on Quality of Life in Terminal Illnesses
Dispelling Common Myths About Palliative and Hospice Care
- There are a lot of misconceptions about palliative and hospice care, which can make it difficult to talk about and accept. Knowing the facts can help people make the best choice for their own or their loved ones’ end-of-life care.
- First of all, it is important to know that neither palliative nor hospice care hastens death, even though they both provide comfort and support to those nearing the end of life. People often fear that hospice services will stop treatments from taking place, but in fact, hospices will provide comfort care that helps to make the patient more comfortable and relaxed, while still allowing treatments to continue.
- Another misconception is that hospice care only takes place in a nursing home or hospital. In fact, most hospice care is provided in the patient's own home. This means that the patient and their family can receive support in the comfort of their own environment.
- Finally, many people think that once you choose palliative or hospice care that there is no going back and that it is a sign of giving up hope. However, this is not true. Healthcare professionals will work with each individual patient and families to adjust the care to fit their needs and will reassess periodically to make sure the care is still meeting their needs.
- It is important to understand the facts about palliative and hospice care to make the best choice for yourself or your loved one. While it can be difficult to talk about and accept, palliative and hospice care can provide comfort and support to those at the end of their life.
- End-of-life care is a difficult topic for many people. It is an emotional time for those who are terminally ill as well as their loved ones. When facing a terminal illness, it is important to both provide physical care and emotional and spiritual support. Emotions can often be overwhelming for those facing difficult end-of-life decisions, which is why it is essential to provide a safe space for them to express their thoughts and feelings.
- Family and friends can play an important role in providing emotional and spiritual support during end-of-life care. Creating a supportive environment by listening to patients, offering comfort and compassion, and respecting a person's wishes can make a huge difference. A strong support system is also necessary for the patient’s caregivers, who may become overwhelmed with the task of caring for a terminally ill loved one.
- Spiritual guidance may also be beneficial for those nearing the end of life. This could involve speaking with a spiritual leader, pastoral counselor, or hospice chaplain to discuss any spiritual matters. This may include facing fear, finding hope, and gaining acceptance of the inevitable.
- Ultimately, providing emotional and spiritual support during end-of-life care is essential in allowing patients and families to address their concerns in a safe and compassionate environment.
- Being a caregiver for a person nearing the end of life can be an emotional and difficult time. To help provide physical and emotional care, there are many organizations and programs available to caregivers in need of assistance.
- Hospice Care Centers: Hospice care centers provide 24-hour medical attention and emotional support. They offer assistance with medical equipment, symptom management, and spiritual guidance.
- Home Health Agencies: Home health agencies can provide medical and personal care services in the patient’s home.
- Caregiver Organizations: Caregiver organizations provide resources and support for those caring for a family member or friend with a chronic illness or disability.
- Support Groups: Support groups are available to discuss end-of-life issues with other caregivers who may be going through similar experiences.
- Financial Assistance Programs: Financial assistance programs offer guidance on how to navigate the financial aspects of end-of-life care. They can also provide resources for accessing financial aid.
- Caregivers will be able to find information and resources through local support groups, hospitals, hospices, and nonprofit organizations.
- The end of life is a difficult time for both patients and their families. Understanding the different options available can help make the experience a little easier. When it comes to palliative care and hospice, it is important to take the time to understand how they differ and how they can both provide unique advantages.
- Palliative care focuses on providing patients with relief from pain and other physical symptoms. It also works to reduce emotional, social, and spiritual stress that may be caused by a terminal diagnosis. Hospice care, on the other hand, is more geared toward helping those who are nearing the end of life. It offers supportive services in order to help make the patient's remaining days as comfortable as possible.
- The key is to explore all options for end-of-life care. By doing so, you’ll be better informed to make decisions for yourself or your loved ones. This means talking to health care professionals and having honest conversations with family and friends. Remember, you don't have to go through this alone.
Exploring the Differences Between Palliative Care and Hospice
Caregiver Resources and Support
Emotional and Spiritual Support at End-of-Life
You might also like this article: